PDF 323 KB
Hepatitis B virus (HBV) causes liver inflammation - spread when infectious body fluids come into contact with body tissues beneath the skin
Infection with the hepatitis B virus (HBV) causes inflammation of the liver.
Hepatitis B is a notifiable condition1
Hepatitis B is spread when infectious body fluids (blood, saliva, semen and vaginal fluid) come into contact with body tissues beneath the skin (for example, through needle puncture or broken skin) or mucous membranes (the thin moist lining of many parts of the body such as the nose, mouth, throat and genitals). In Australia the most likely ways people will have become infected are:
Other ways of contracting hepatitis B include:
The risk of spread is increased when there are higher levels of virus in the blood. The level of virus varies considerably between people infected with hepatitis B.
(infection usually lasts than 6 months)
About 50% of adults and 90% of children do not develop any symptoms at the time of infection.
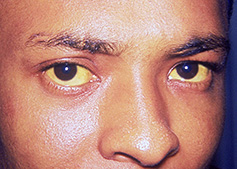 Symptoms, if they occur, may include:
Symptoms, if they occur, may include:
Acute infection may be followed by chronic infection (long lasting). People unable to eliminate the hepatitis B virus from their body following an acute infection and who remain infected for more than 6 months are said to have chronic hepatitis B infection.
Image Courtesy Public Health Image Library (PHIL), Department of Health and Human Services, Centers for Disease Control and Prevention (CDC-USA) CDC,Dr. Thomas F. Sellers / Emory University
Risks for developing chronic infection are age and immune deficiency. With age,
Most people chronically infected with hepatitis B have no symptoms but are capable of spreading the infection to others. People chronically infected with hepatitis B have an increased risk of developing cirrhosis (scarring) of the liver and liver cancer later in life.
Both acute and chronic hepatitis B infections are diagnosed by blood tests serology and PCR (polymerase chain reaction) tests in a pathology laboratory.
If liver inflammation continues, a needle may be inserted into the liver to obtain a sample of liver for further testing.
(time between becoming infected and developing symptoms)
Between 45 to 180 days, and rarely from as early as 2 weeks to as late as 9 months.
(time during which an infected person can infect others)
From up to 3 months before symptoms develop until the infected person eliminates the virus from their body. Chronically infected people remain infectious for life although the risk of transmitting the infection to others varies considerably from person-to-person.
Antiviral treatment is available and is of benefit to some people with chronic hepatitis B infection.
People with hepatitis B virus infection but no symptoms were once thought to be 'healthy carriers'. However, all people with chronic hepatitis B should receive regular, lifelong monitoring of disease progression by a general practitioner or liver specialist .
Routine monitoring (at least annually) even when there are no symptoms, can prevent severe liver disease including liver cancer.
There is a safe and effective vaccine available for hepatitis B for infants and those at higher risk of acquiring hepatitis B infection and/or higher risk of severe disease. Completion of a full course will give protection against hepatitis B infection in more than 90% of people. See the Australian Government's Hepatitis B vaccine page or the SA Health High Risk Hepatitis B Immunisation Program for more information. A combination hepatitis A and B vaccine is available and should be considered for:
Hepatitis B vaccine and/or immunoglobulin can be given soon after exposure to make it less likely a person will develop hepatitis B. This is called post exposure prophylaxis.
Read the Get tested, get vaccinated, eliminate Hepatitis B infographic for more information.
Hepatitis B immunoglobulin is a solution made from blood products containing a high level of antibodies specific to the hepatitis B virus.
Hepatitis B immunoglobulin and vaccine are also offered to non-immune people who have had close physical contact with a person known to be infected with hepatitis B in the following situations:
Immunoglobulin is offered after needle stick injuries unless the source is known to be negative for hepatitis B. Immunoglobulin should be administered as soon as possible within 72 hours after a needle stick injury and within 14 days after sexual exposure.
All women are tested for hepatitis B infection during pregnancy. If a mother is found to have hepatitis B infection, her baby is given immunoglobulin and a dose of hepatitis B vaccine within 24 hours of birth. With this treatment less than 10% of infants become infected with hepatitis B.
1 – In South Australia the law requires doctors and laboratories to report some infections or diseases to SA Health. These infections or diseases are commonly referred to as 'notifiable conditions'.